Donor Egg + Genomics
![]()
![]()
At ORM we are proud of our commitment to comprehensive donor screening, combining the latest genomic technologies with the clinical expertise of our genetic counseling team. Please see our main ORM Donor page for background information on our donor program.
ORM recognizes the importance of two very different but complementary genetic screening strategies for egg donors: (1) genetic carrier screening, and (2) assessment of the donor’s family history. Each provides essential information about genetic risks that cannot be uncovered by the other. After embryos are created, comprehensive chromosome screening can give us valuable information about the health and viability of the embryos.

Carrier Screening
What We Do
All ORM egg donor applicants have expanded genetic carrier screening for > 150 recessive conditions(1) on the Counsyl Family Prep Screen. This screening is significantly more extensive than the standard practice of many clinics and agencies, and also includes a number of X-linked conditions(2). It is common to be a carrier of recessive genetic diseases – about 60% of individuals who have the Counsyl Family Prep Screen will be found to be a carrier of at least one condition. Most carriers have no family history of a genetic disease and would only have learned that they are a carrier if a child with the disease was born.
The ORM difference:
Genetic carrier screening before matching.
All ORM egg donors have carrier screening before they are ever placed on our donor database. In most instances, women who are carriers of recessive conditions are still eligible to be egg donors. But having the donor’s carrier screen results available to you from the start allows you to avoid matching with a donor who is later discovered to be a carrier of the same condition as the sperm provider, causing the match to be cancelled. Advance carrier screening also reduces the chance that you will match with a donor who is later determined to be ineligible due to her carrier screening results. Donor applicants who are carriers of recessive conditions associated with personal health risks to carriers, or of X-linked conditions, are excluded from being ORM donors due to the increased health risks to genetic offspring.

Family History Genetic Consultation
What We Do
- All ORM egg donor applicants complete an extensive family history questionnaire which is reviewed by the donor intake coordinator. A stringent set of exclusion criteria are applied up-front to exclude egg donors with a significant personal or family history of a number of severe health conditions, birth defects, and mental illness.
- While everyone has an increased risk for certain health problems based on their family history, ORM strives to reduce the risk for genetic diseases and serious health problems in donor-conceived offspring. Therefore, egg donors who pass the initial exclusion criteria have a 30-minute consultation with an ORM in-house certified genetic counselor to review their family history in detail. The genetic counselor obtains a complete three-generation family history and asks follow-up questions to clarify diagnoses, ages of onset, environmental contributors, and potential patterns within the family. Genetic counselors are expertly trained to assess family histories for the presence of major genetic diseases (such as autosomal dominant conditions5), which may go unnoticed in a questionnaire because they may have different features and levels of severity within a family. The genetic counselor will also assess the presence of common health problems with a familial/genetic component, such as heart disease, cancer, diabetes, and mental illness. We have developed our own donor exclusion criteria by following and expanding upon the recommendations for gamete donor screening by the American Society of Reproductive Medicine.
- Once an egg donor applicant has been formally accepted as an ORM donor, the genetic counselor completes a comprehensive Genetic Information and Family Tree [GIFT] summary. This assessment is available to help you interpret the genetic risks present in a donor’s family history, which may be helpful during your donor selection process. Importantly, the GIFT summary also provides a record of the donor’s family medical history that can eventually be shared with your child and their health care providers to enable appropriate medical care and screening in the future.
The ORM Difference:
Why is review by a genetic counselor important?
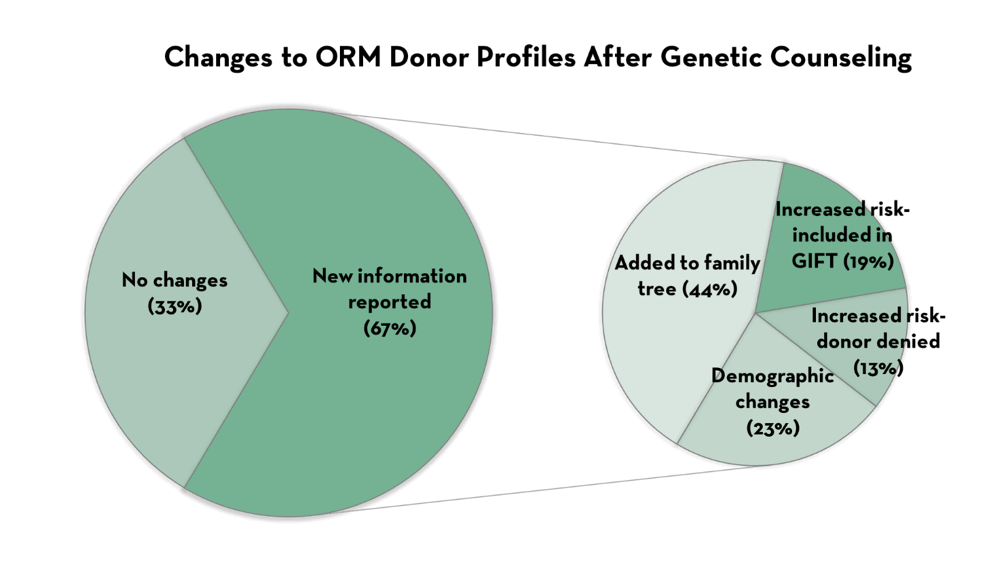
A review of over 400 egg donor applicants to ORM found that consultation with one of our genetic counselors uncovered new family history information (a health problem or a diagnosis that was not previously reported on the screening questionnaire) for over 50% of egg donor applicants. In over 30% of these cases, the new information was associated with an increased risk for the donor’s genetic offspring to develop a health problem, and many of these donors were then excluded from the program. It is important to remember that the vast majority of concerns uncovered by a thorough family history are NOT detected by blood genetic carrier screening. The comprehensive family history review is a unique service at ORM, and is not offered by most egg donor agencies.

Comprehensive Chromosome Screening in Embryos from Donor Eggs
If you are using donor eggs to start your family, we will offer to perform comprehensive chromosome screening (CCS) on your embryos using the most advanced technology, next-generation sequencing, in our in-house NGS lab. While chromosome problems are most common in embryos created using the eggs of older women, at ORM we have found that 1 in 3 embryos created from donor eggs (age 21-29) have chromosome abnormalities discovered on CCS. These embryos would not have been able to make a healthy baby due to a randomly-occurring chromosome problem. Using CCS to select the best embryos for transfer will in some cases improve the pregnancy rate, decrease the chance of a miscarriage occurring, and reduce the chance that the baby has a chromosomal condition such as Down syndrome. At ORM over 90% of our donor egg IVF patients now choose to do CCS with a frozen embryo transfer.
Footnotes
1. Recessive inheritance
We typically have two copies of every gene, one from the egg provider and one from the sperm provider. Carriers of a recessive genetic disorder have a mutation in one copy of a particular gene, which causes that gene to not work correctly. However, because the other copy of that gene is working fine, carriers are usually healthy and have no signs of the disorder. If someone inherits two non-working copies of the same gene, they could have a genetic disease. If an egg donor and the sperm provider are carriers of mutations in the same gene, there is a 25% chance for the offspring to have that disorder due to recessive inheritance. Return to content ↩
2. X-linked inheritance
X-linked conditions are caused by mutations in genes on the X chromosome 4. Females typically have two X chromosomes (XX) and males typically have one X chromosome and one Y chromosome (XY). Males are more likely to be affected by non-working genes on the X chromosome because they only have one copy of most of those genes. Females have two copies of the genes on the X chromosome, and therefore females can be carriers of X-linked conditions. Female carriers of X-linked conditions have an increased chance to have male children affected with that genetic condition. Female carriers are often healthy, however some develop symptoms of that condition, particularly as they age. Return to content ↩
3. Genes
Genes are a set of instructions that influence and direct development, health, and appearance by coding for important proteins and enzymes. Genes are made up of DNA, and are passed on from generation to generation. It is thought that humans have about 20,000 genes. Sometimes genes can have spelling mistakes, or mutations, that change the type of protein a gene makes, or stops it from making that protein entirely. Mutations in genes can affect normal health and development. Return to content ↩
4. Chromosome
Chromosomes are packages of genes, or DNA, within the cells. Humans normally have 46 chromosomes in each cell; 23 come from the sperm cell and 23 from the egg cell. The first 22 pairs of chromosomes are identified by number, 1 through 22, while the last pair reflects the sex of the embryo: XX for female, XY for male. Return to content ↩
5. Autosomal dominant
We typically have two copies of every gene3, one from the egg provider and one from the sperm provider. Carriers of a dominant genetic disorder have a mutation in one copy of a particular gene, which causes that gene to not work correctly. Although they have a second working copy of that gene, it is not enough to prevent them from developing that health condition. If an egg provider or sperm provider have a dominant genetic condition, there would be a 50% chance for each genetic offspring to inherit that condition. Many dominant genetic conditions can be difficult to detect, as there can be significant variability in severity and age of onset, even within family members. Some dominant conditions also have reduced penetrance, which means that not everyone that inherits the faulty gene will develop the condition. Return to content ↩
